Have you ever seen someone with missing teeth? Did you notice the way their face looks slightly sunken in, almost as if they’re constantly sucking on a lemon? That person was almost certainly dealing with bone loss.
Bone loss can happen to anyone — it’s not only associated with age. Bone loss can stem from many causes, including improper oral care and other lifestyle factors. Keep reading to learn more about the symptoms associated with bone loss, what can be done to prevent it, and treatment options.
What is dental bone loss?
Maintaining healthy teeth is an important part of sustaining our overall long-term health. Our natural teeth work to stimulate bone growth and preserve bone through chewing and biting. When you’re missing a tooth, the bone no longer gets this stimulation, causing the bone to disintegrate, a process known as resorption.
Advanced gum disease can also eat away at your jawbone, causing bone loss and ultimately leading to tooth loss. Once you’ve lost a tooth, additional bone and tooth loss are likely.
What causes bone loss in the jaw?
Bone loss can occur for a number of reasons. Find the most common ones below.
Tooth Extractions
The most common cause of bone loss is tooth extraction.
The jawbone is preserved through activities like chewing and biting. When an adult tooth is removed and not replaced, jaw bone deterioration begins. In the first year after tooth extraction 25% of bone is lost, and this bone loss continues with time. When teeth are missing, the alveolar bone, or the portion of the jaw bone that anchors the teeth in the mouth, no longer receives the necessary stimulation and begins to break down, or resorb. The body no longer uses or needs the jaw bone, so it deteriorates.
Gingivitis
Dental plaque is the primary cause of gingivitis. Plaque is a sticky colorless film that adheres to your teeth at and below the gum line. When daily teeth brushing and flossing is neglected, the plaque can harden and cause your gums to become inflamed, red, swollen, and bleed easily.
Periodontitis
Also known as gum disease, periodontal diseases are ongoing infections of the gums that cause damage to the soft tissue and bone that support your teeth. Plaque-induced inflammatory lesions make up the majority of periodontal issues and are divided into two categories: gingivitis and periodontitis. Even though gingivitis is the less serious disease, it always precedes periodontitis.
Periodontitis is affected by bacteria that adheres to the tooth’s surface, along with an overly aggressive immune response to these bacteria. If gingivitis progresses into periodontitis, the supporting gum tissue and bone that hold teeth in place deteriorates. The progressive loss of this bone can lead to the loosening and loss of teeth.
Dentures/Bridgework
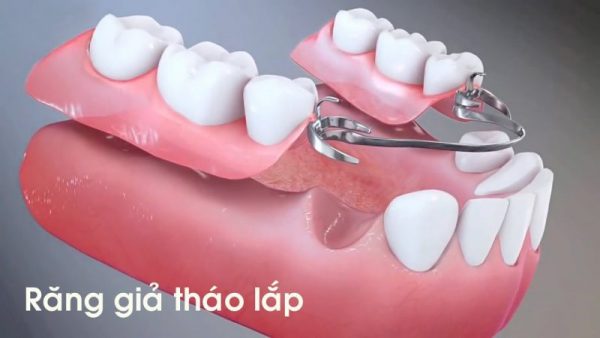
Wearing anchored dentures may increase the rate at which the bone deteriorates. This type of denture is placed on top of the gum line, but does not provide any direct stimulation to the underlying alveolar bone. With time, the bone deteriorates due to lack of stimulation and causes loosening of the dentures and problems eating and speaking. If your dentures begin to loosen, they might require refitting.
Wearing removable dentures for a long time leads to severe jaw bone loss
However, Some dentures preserve the bone because they are supported by anchors, which stimulate the alveolar bone.
Bone loss can occur with bridgework because the portion of the bridge that spans the gap where the teeth are missing receives no direct stimulation from chewing.
By completing a bone graft procedure, Dr. Bauer is now able to restore bone function and growth, thereby halting the effects of poor denture care.
Facial Trauma
When facial trauma occurs, like when a tooth is severely damaged or knocked out and no biting surface remains, it results in jaw bone loss.
A bone grafting procedure provides the opportunity to not only replace bone where it is missing, but also the ability to promote new bone growth in that location. This process will reverse the effects of bone deterioration, restoring function and promoting new bone growth in traumatized areas.
Misalignment
Jaw misalignment can create situations where some teeth no longer have opposing tooth structure. Over time, bone deterioration can occur where the bone is losing stimulation. Issues such as TMJ problems, normal wear-and-tear, and lack of treatment can also contribute to jaw bone deterioration.
Osteomyelitis
Osteomyelitis, a type of bacterial infection in the jawbone (maxilla and mandible) and its bone marrow, leads to inflammation, which can result in blood loss to the bone. Treatment for osteomyelitis generally requires antibiotics and the removal of the affected bone.
Tumors and cancer
Large benign facial tumors might need to be removed. Although they are generally not life-threatening, they can be aggressive enough to invade nearby tissue and bone, repositioning teeth, and causing long-term damage to your face and neck.
Cancerous tumors typically spread through the jaw and require removal of the affected section.
Jawbone reconstruction is usually required in both cases to restore proper functionality. Bone grafting is a treatment option for both, but may be more challenging in patients with malignant tumors because treatment of the cancerous tumor generally requires removal of the surrounding soft tissues.
Developmental Deformities
Jawbone loss can occur due to developmental deformities (birth defects) resulting in missing portions of teeth, facial bones and skull.
Sinus Deficiencies
The bones in your face and jaw help to keep your teeth in place. When molars from the top of your mouth are removed, air pressure from the air cavity in your sinus causes resorption of that bone. Sinuses then become enlarged over time and result in insufficient bone.
Symptoms of bone loss
Patients affected by bone loss often suffer from additional issues related to their dental health. Here are the symptoms you’re most likely to experience due to bone loss:
- Changes in your bite and facial structure. If you wear dentures, bone loss can cause changes in the overall fit and comfort (i.e. they can feel loose or fit differently).
- Discomfort when you chew
- Shifting or loosening of your teeth
- Shrinking gums
- Lips beginning to sink inward
- Headaches, facial pain, and jaw pain
- Increased difficulty speaking
- Loose teeth
- New gaps between your teeth
- Bad breath
- Pain when chewing
Can you reverse bone loss in the jaw?
We always recommend preventing bone loss in the first place. Here’s how:
- Replace missing teeth as soon as you lose them.
- Practice good everyday oral hygiene habits.
- Stay up to date with your routine dental cleanings and exams.
- Follow all your dentist-recommended treatment or prevention plans.
- If you are already suffering from bone loss, thankfully treatment options do exist and are very successful.
Treating bone loss
Effective treatments for bone loss in the jaw include the following:
Guided Bone Regeneration
This treatment rebuilds the bone that’s been lost, creating an adequate, strong, and stable foundation to replace a missing tooth.
Bone Graft
Bone grafting – The most common treatment for jawbone atrophy is a bone graft. This procedure can repair implant sites with inadequate bone structure due to previous extractions, gum disease, or injuries. It also provides the opportunity to place dental implants and restore functionality and aesthetic appearance where it was not previously possible.
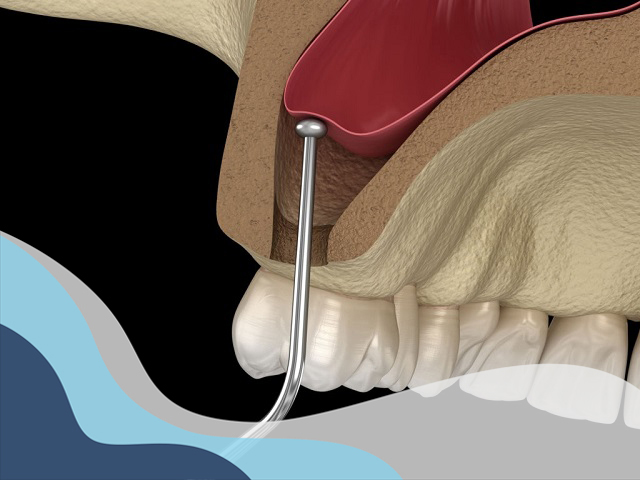
Sinus lift – Dr. Tuan can lift the sinus cavity by positioning its membrane lining away from the jaw and introducing bone graft material into the area. This enables dental implants to be placed and institute bone growth.
Replacing missing teeth with an implant
Once your bone is strong enough to support an implant, we highly recommend replacing any missing teeth. This will help support your jaw bone and prevent any additional tooth loss in neighboring teeth.